10
Jul

9 Unexpected But Exciting Side Effects of Weight Loss
Whether from GLP-1 or other medical weight loss solutions, as the number on the scale declines, you're likely to experience some unexpected but exciting side effects! Side effects are often referred to as negative, but they can be positive too. From increased energy to conf...
View More02
Jul

Skin SOS: Tips to Avoid Summer Sun Damage
We want you to get out and enjoy the Arizona summer, but we also want you to be safe! In addition to hydrating your body, you must protect your skin from the sun's UVA and UVB rays. Sun damage doesn’t just increase your risk of skin cancer, it breaks down collagen and...
View More25
Jun
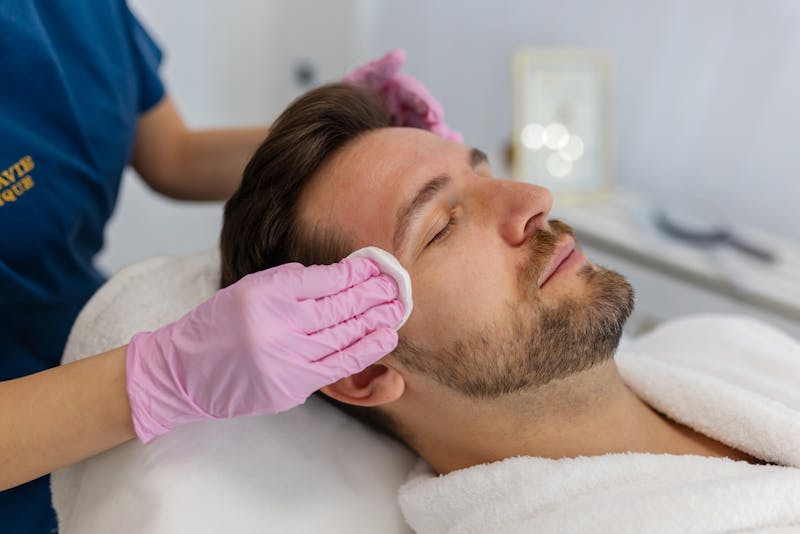
Top 5 Med Spa Treatments For Men
Women aren't the only ones looking for non-surgical methods of slowing aging and improving their appearance. Yes, we call it “distinguished” when men display fine lines, but men experience ageism and insecurities too. Valley Medical Weight Loss and Med Spa is he...
View More19
Jun

How to Meal Plan Like a Pro!
It doesn't matter what we’re referring to, having a plan saves time, minimizes stress, and increases the likelihood of success. This approach rings true when mapping out your weekly recipes. We understand how busy you are and that you may be planning meals for family...
View More11
Jun

Hydration Tips: Staying Hydrated in Arizona This Summer
Arizona summers are the best time of the year, but the heat is extreme. The more time you spend outside and the more rigorous the activity, the more important it is to hydrate your body. Increasing your water intake, consuming hydrating foods, and increasing electrolytes reduces...
View More04
Jun

Emotional Eating: How to Manage When Stress and Emotions Are High
We've all been there. We’re sad, stressed, or lonely, and we “eat our feelings”. Emotional eating isn’t a sheer matter of willpower. It’s a coping mechanism, and fast and easy way to feel better or gain a sense of control when emotions are high...
View More29
May

Inflammaging Skincare: Are You Accidentally Inflaming and Aging Your Skin?
In an effort to keep your skin wrinkle-free, you may have unknowingly adopted a few skincare and beauty habits that do more damage than good. This can span the range of applying topical products that work initially, but damage skin over the long term. Or misusing topical products...
View More22
May

Health Beyond The Scale: You Achieved Your Goal Weight, Now What?
Congratulations! You've achieved your goal weight or are on your way. Now you might be wondering what’s next? It’s time to consider what this powerful new body of yours can do that it couldn’t do before. Also, what the next personal or professional goal yo...
View More14
May

9 Tips For Getting Summer Body Ready
Getting summer body ready, isn't just about losing weight. It’s about ensuring you feel your best inside and out. In fact, you may not have any weight to lose! Either way, you’ll need to make a few changes to your skincare routine, nutrition, and lifestyle to ma...
View More07
May

Managing Perimenopause: How to Thrive as You Enter Your Next Phase of Life!
Life isn't over in perimenopause or postmenopause! In fact, many women feel more confident with age and define this season of life as one of the most empowering. Much of this confidence comes with dispelling menopause myths and removing the stigmas associated with this tran...
View More
